Our skin is the body’s largest organ and its first line of defense against the environment. From sun exposure and pollution to stress and diet, many factors can affect skin health. It’s no surprise that millions of people worldwide struggle with common skin conditions at some point in their lives. While some are temporary and mild, others may require ongoing care or medical attention. Knowing how to identify, prevent, and safely treat these conditions can help you maintain healthy, glowing skin.
In this blog, we’ll explore the most common skin conditions and provide safe treatment tips for each.
ACNE
Acne is one of the most common skin concerns, affecting both teenagers and adults. It occurs when hair follicles become clogged with oil, dead skin cells, and bacteria, leading to pimples, blackheads, or cysts.
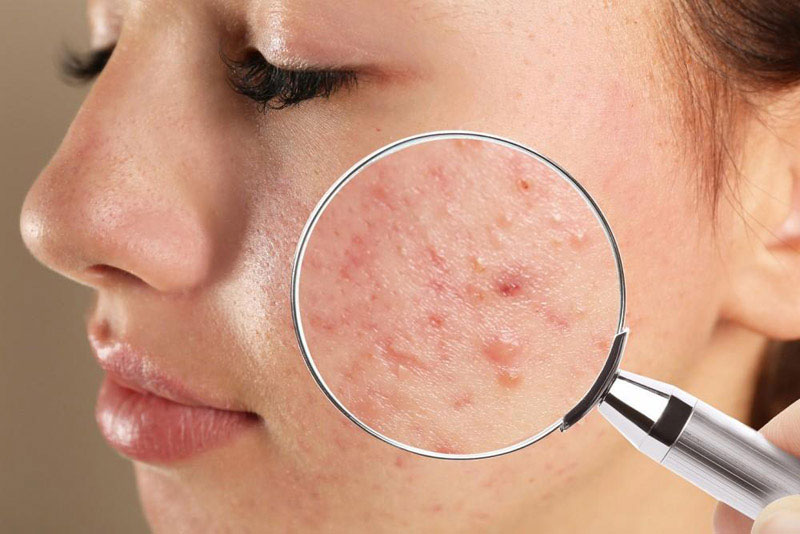
Causes:
- Excess oil production
- Hormonal changes (puberty, pregnancy, menstruation)
- Stress and poor diet
- Use of heavy skincare or makeup products
Safe Treatments:
- Use gentle, non-comedogenic cleansers.
- Apply topical treatments with ingredients like benzoyl peroxide or salicylic acid.
- Avoid picking or squeezing pimples to prevent scarring.
- For severe acne, consult a dermatologist for prescription medications or therapies.
ECZEMA (Atopic Dermatitis)
Eczema is a chronic skin condition that causes red, itchy, inflamed patches. It often appears in children but can affect people of all ages.
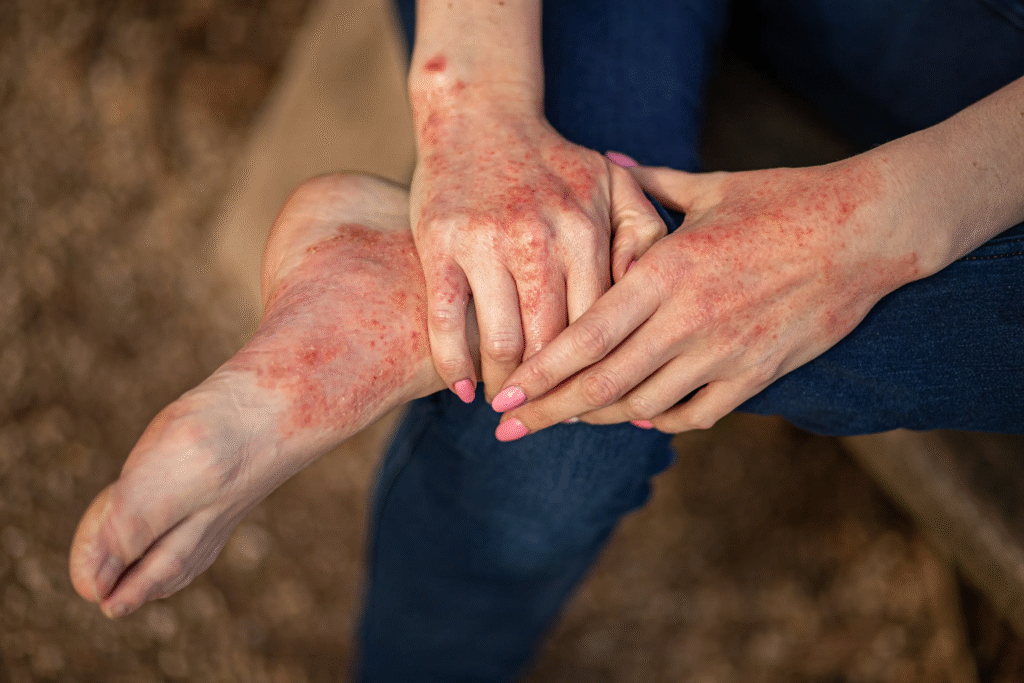
Causes:
- Overactive immune system
- Allergies
- Genetics
- Environmental triggers like soaps, detergents, or pollen
Safe Treatments:
- Keep the skin moisturized with fragrance-free creams.
- Use mild, hypoallergenic soaps and detergents.
- Avoid scratching to reduce infection risk.
- In persistent cases, doctors may recommend topical corticosteroids or other medicated creams.
PSORIASIS
Psoriasis is an autoimmune condition that speeds up skin cell turnover, resulting in thick, scaly patches on the skin.

Causes:
- Immune system overactivity
- Genetics
- Triggers such as stress, infections, or cold weather
Safe Treatments:
- Moisturize daily to reduce dryness and scaling.
- Apply medicated creams containing coal tar or salicylic acid.
- Light therapy (under medical guidance) can help in certain cases.
- Severe psoriasis may require oral or injectable medications prescribed by a dermatologist.
ROSACEA
Rosacea causes redness, visible blood vessels, and sometimes acne-like bumps, often on the face.
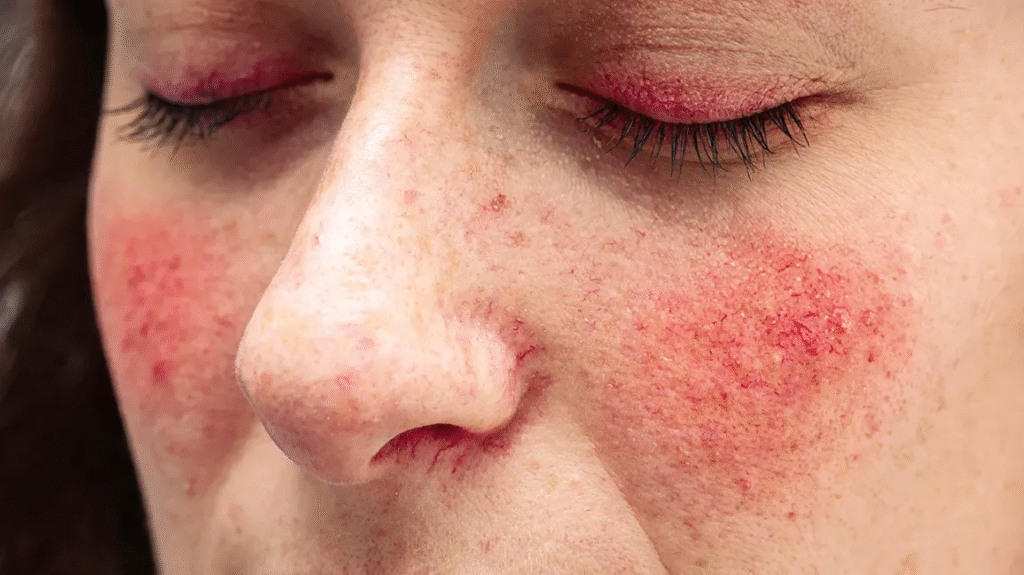
Causes:
- Exact cause unknown, but linked to genetics, immune response, and environmental triggers
- Common triggers: spicy foods, alcohol, hot drinks, sun, stress, and heat
Safe Treatments:
- Identify and avoid personal triggers.
- Use gentle skincare products designed for sensitive skin.
- Protect skin from sun exposure with broad-spectrum sunscreen.
- Dermatologists may prescribe topical creams or oral antibiotics for flare-ups.
FUNGAL INFECTION (Ringworm, Athlete’s Foot, Yeast Infections)
Fungal infections can affect various parts of the body, causing itchy, red, and sometimes scaly rashes.
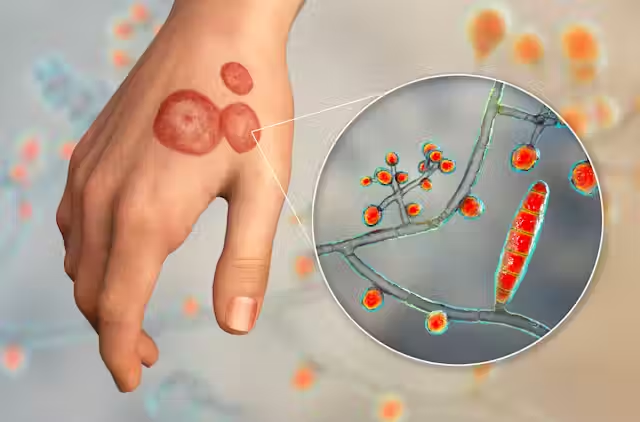
Causes:
- Warm, moist environments
- Poor hygiene
- Sharing contaminated items like towels or shoes
Safe Treatments:
- Keep skin clean and dry.
- Use over-the-counter antifungal creams or powders.
- Wear breathable fabrics and avoid tight clothing.
- Severe or recurring infections may need prescription antifungal medications.
CONTECT DERMATITIS
This occurs when the skin reacts to irritants or allergens, leading to redness, swelling, and itching.
Causes:
- Harsh chemicals, soaps, or detergents
- Nickel in jewelry
- Cosmetics or fragrances
- Poison ivy and other plants
Safe Treatments:
- Identify and avoid the irritant or allergen.
- Soothe skin with cool compresses and fragrance-free moisturizers.
- Over-the-counter hydrocortisone creams may reduce inflammation.
- Seek medical help if symptoms persist or worsen.
HIVES (Urticaria)
Hives are itchy, red welts that appear suddenly and may come and go within hours or days.
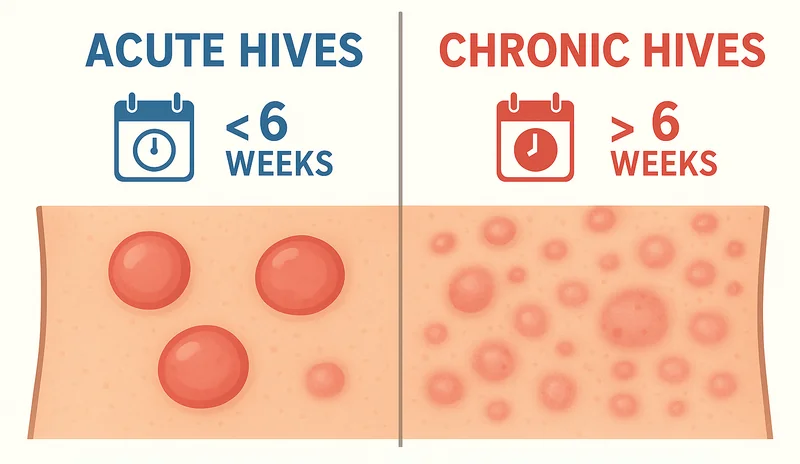
Causes of Acute Hives:
- Food Allergies: Common culprits include shellfish, nuts, eggs, and dairy.
- Medications: Antibiotics, aspirin, ibuprofen, and other pain relievers.
- Insect Bites or Stings: Mosquitoes, bees, and wasps may trigger sudden hives.
- Infections: Viral infections like the flu or bacterial infections like strep throat.
- Environmental Factors: Cold air, heat, pollen, or pet dander.
Symptoms of Acute Hives:
- Red, raised welts on the skin
- Intense itching or burning sensation
- Sudden onset, often within minutes to hours of exposure
- Possible swelling in lips, eyelids, or throat (angioedema)
Treatment for Acute Hives:
- Antihistamines: Over-the-counter antihistamines like cetirizine or loratadine can reduce itching.
- Avoiding Triggers: Identifying and eliminating the cause is essential for quick recovery.
- Topical Relief: Cool compresses or soothing lotions can ease discomfort.
- Emergency Care: If hives are accompanied by difficulty breathing, dizziness, or swelling of the throat, seek immediate medical help as it could be a sign of anaphylaxis.
Causes of Chronic Hives:
Unlike acute hives, chronic hives are not always linked to an obvious trigger. Possible causes include:
- Autoimmune Disorders: The body mistakenly attacks its own tissues, triggering hives.
- Underlying Medical Conditions: Thyroid disease, lupus, and other immune system issues.
- Chronic Infections: Hepatitis, urinary tract infections, or sinus infections.
- Stress and Hormones: Psychological stress, menstrual cycles, or hormonal imbalances may worsen symptoms.
- Idiopathic: In many cases, no clear cause is found (chronic idiopathic urticaria).
Symptoms of Chronic Hives:
- Persistent or recurring itchy welts for weeks or months
- Welts may change shape, size, and location throughout the day
- Swelling in deeper layers of the skin (angioedema)
- Severe itching that interferes with sleep and daily life
Treatment for Chronic Hives:
- Long-Term Antihistamines: Daily non-drowsy antihistamines prescribed by doctors.
- Advanced Medications: In resistant cases, drugs like omalizumab (a biologic therapy) or corticosteroids may be prescribed.
- Lifestyle Management: Stress reduction techniques, dietary adjustments, and avoiding alcohol or known irritants.
- Regular Monitoring: Since chronic hives may be linked to autoimmune conditions, ongoing medical checkups are important.
WARTS
Warts are small, rough skin growths caused by human papillomavirus (HPV). They are contagious and can spread through skin contact.
Causes:
- HPV infection
- Direct contact with infected surfaces or skin
Safe Treatments:
- Over-the-counter salicylic acid treatments
- Freezing (cryotherapy) by a healthcare provider
- Avoid picking warts to prevent spreading
General Skin Care Tips for Prevention
- Maintain Good Hygiene: Wash your face and body regularly with mild cleansers.
- Stay Hydrated: Drink plenty of water to keep skin moisturized.
- Eat a Balanced Diet: Nutrient-rich foods support skin repair and protection.
- Sun Protection: Always use sunscreen with at least SPF 30.
- Avoid Harsh Products: Choose skincare products that are gentle and fragrance-free.
- Consult a Dermatologist: For persistent or severe conditions, professional guidance is essential.
